Why hantavirus isn't the next COVID
A plain-language explainer on the MV Hondius hantavirus outbreak — what actually happened, why the WHO calls overall risk "low," and what the bigger picture means for your actual health priorities.
Your phone is full of hantavirus news right now. A cruise ship. Seven confirmed infections. Three deaths. A Reddit post from 2012 went viral again. TikTok is full of people strapping masks on at airports and joking about buying toilet paper. And somewhere in all the noise, a totally reasonable question has gotten lost: should I actually be worried?
Short answer: no — not in any meaningful way.
Longer answer: here's what's actually going on, why this virus behaves nothing like COVID, and what the whole thing reveals about where public health infrastructure is right now.

What's happening on that ship
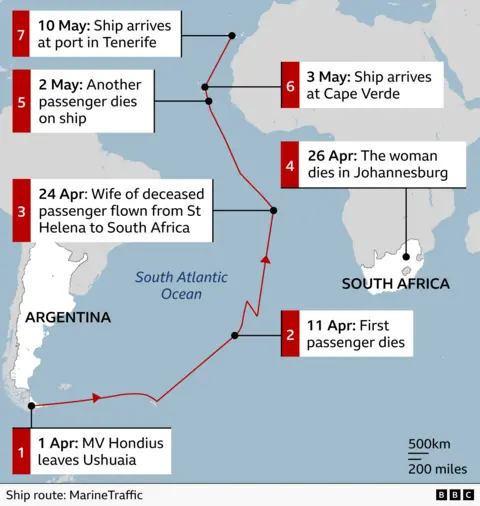
The MV Hondius is a Dutch-flagged polar expedition vessel operated by Oceanwide Expeditions. 1 It left Ushuaia, Argentina on April 1 carrying 147 people — 86 to 88 passengers and 59 to 61 crew from 23 nationalities — headed on a South Atlantic expedition route through Antarctica, South Georgia, Tristan da Cunha, St. Helena, and Ascension Island.
The first person to get sick was an adult Dutch male passenger who developed fever, headache, and diarrhea on April 6. He died April 11 onboard. He was never tested. His wife fell ill shortly after; she left the ship at St. Helena on April 24, flew to Johannesburg, and died there on April 26. Her samples came back PCR-positive for Andes hantavirus on May 4. 2
From there, the outbreak unfolded across thousands of miles of ocean. A third patient was medically evacuated from Ascension Island on April 27 to a South African ICU. A fourth — an adult German woman — died onboard May 2 with pneumonia symptoms. The WHO was notified by the UK on May 2 and published a full disease outbreak notice on May 4. 1
As of May 11, the count stood at 7 confirmed cases (including an American passenger and a French woman now in Paris), 2 suspected, 3 deaths, with the ship evacuated at Tenerife in the Canary Islands. Multiple countries — the US, UK, Spain, and others — repatriated their citizens under varying quarantine protocols. The CDC deployed a team and sent American passengers to the Nebraska Medical Center for a 42-day monitoring period. 3
This is a real, serious outbreak. It killed three people. It also, critically, happened on a single ship in a very specific context — and that context matters a lot.
What hantavirus actually is
Hantaviruses are a family of rodent-borne viruses that have been around for a long time. 4 The family was first identified and named after the Hantan River in Korea, where it caused illness in troops during the Korean War. These are not new viruses suddenly emerging from the deep — they've been studied for decades.
The primary route of infection is pretty specific: you inhale tiny aerosolized particles from infected rodent urine, droppings, or saliva. Think cleaning out an old cabin, sweeping a dusty barn, or disturbing a nest in a wall. Touching a contaminated surface and then touching your face can also do it.
The virus that's in the news right now — Andes virus — is unusual. Out of all the hantavirus species known to science, the Andes virus is the only one documented to spread person-to-person. 5 Even then, it doesn't spread easily. The WHO has been explicit: transmission requires "close and prolonged contact, particularly among household members, intimate partners and people providing medical care." Casual contact, shared air in a room, a conversation at a bar — none of that is how Andes virus gets from one person to another.
Once you're infected, the incubation period is 4 to 42 days. Early symptoms look almost exactly like the flu: fever, fatigue, muscle aches in the large muscle groups (thighs, hips, back), headache, nausea, vomiting, diarrhea. Then, in severe cases, the virus progresses to Hantavirus Pulmonary Syndrome (HPS) — fluid builds up in the lungs, breathing becomes extremely difficult, and the body goes into shock. The CDC estimates a roughly 38% case fatality rate among patients who develop those respiratory symptoms. 3 That number sounds terrifying — and for people who reach that stage, it absolutely is. But as Dr. Jeanne Marrazzo, CEO of the Infectious Diseases Society of America, noted: "While those are very scary numbers, we often don't know what the denominator of people infected is, because mild cases might be missed." 4 In other words, the 38% likely overcounts severity because mild cases don't make it into the statistics.
To put the US scale in perspective: there have been 890 confirmed hantavirus cases in America over the past 30 years. Most were in rural western states at higher elevations, where deer mice — the primary carrier in the US — live. 3 The US strain (Sin Nombre virus) does not spread person-to-person at all. The Andes-carrying rodents from Argentina don't live here.
Should you actually be worried?
Here's the WHO's direct assessment: risk to the general global population from this event is low. 1 Maria Van Kerkhove, the WHO's Director of Epidemic and Pandemic Management, said this clearly: "Most people will never be exposed to this." 6 She also wanted to preempt the inevitable comparison: "I want to be unequivocal here. This is not the start of a COVID pandemic." 4
Why is this so different from COVID?
Several reasons. COVID spread before people felt sick, making it almost impossible to contain early. Hantavirus patients deteriorate fast and become visibly ill quickly, which actually limits spread. As Dr. Abraar Karan from Stanford put it, the window of contagiousness is short because patients deteriorate quickly — in a matter of days — leading to isolation or death before they can unknowingly infect many others. 4 Dr. Dean Blumberg at UC Davis noted that on average, infected people spread the virus to fewer than one other person — meaning "outbreaks tend to die out quickly rather than grow." 7
There is no community transmission anywhere right now — not in the US, not in Europe, not in South America (outside the known endemic rodent zones in Argentina and Chile). This is a contained cluster tied to a single ship.
Now about the social media panic: a Reddit post in r/oddlyterrifying showed a 2012 tweet about hantavirus going viral again. 8 TikTok filled with mask-at-airport content. The BMJ reported people are literally betting on whether this escalates to a pandemic. This isn't really about hantavirus — it's about COVID-era anxiety that never fully went away. Someone on Reddit's r/NoStupidQuestions put it plainly: "This is what people are missing. We've been dealing with this for decades. It's not new." 8
Your actual risk assessment as a young healthy adult in the US: essentially zero, unless you were on that specific cruise ship. General hantavirus risk in the US exists only if you're disturbing rodent nests in rural western environments. If you're ever doing that — cleaning out a dusty old cabin, sweeping a barn, working in agricultural settings with potential rodent exposure — ventilate first, don't sweep or vacuum (that aerosolizes particles), wet-mop with a bleach solution, and wear gloves plus a respirator mask.
There's no vaccine and no cure — that part is real
This is the one piece of the hantavirus story that should make you think. There is no licensed hantavirus vaccine anywhere in the world. No specific antiviral drug has been approved for Hantavirus Pulmonary Syndrome. Treatment is entirely supportive: oxygen, mechanical ventilation, ECMO (a life support machine that does the work of the heart and lungs when they fail) in severe cases, careful fluid management. 9
It's not like no one has tried. Researchers at the US Army Medical Research Institute (USAMRIID) completed Phase I trials of a DNA vaccine targeting Andes virus. The science worked at that stage. But Phase II and III trials haven't been funded — there's no obvious population large enough and geographically concentrated enough to run a proper efficacy trial, since cases are rare and scattered. 10
A UK biotech called EnsiliTech has an mRNA vaccine targeting a different hantavirus strain in preclinical stages — the technology would allow room-temperature storage, which matters for distributing it in the remote rural areas where people actually get infected. But they're 3 to 4 years from first human trials. Moderna has early-stage research on hantaviruses with USAMRIID and Korea University, which predates this outbreak. 11
Why hasn't more happened? Sabra Klein at Johns Hopkins Bloomberg School said it directly: "Our funding agencies don't put a lot of money into this, because it's likely not to cause the next epidemic or pandemic." 10 Matt Slade, co-founder of EnsiliTech, put it even more bluntly: "Unfortunately, hantaviruses tend to be endemic in parts of the world that don't really have that financial backing, so I think there's just been a lack of interest." 10 And Dr. Ofer Levy at Boston Children's Hospital summed up the systemic failure: "There has been no 'Warp Speed' for hantavirus." 10
That's a real, legitimate frustration — and a pattern worth knowing about. Diseases that kill people in poor, rural, or low-profile populations don't attract commercial vaccine investment. The cruise ship outbreak might generate some renewed attention. It probably won't generate the hundreds of millions of dollars needed to push a candidate through Phase III.
The bigger picture nobody wants to talk about
Here's the part that's worth sitting with after the hantavirus panic fades.
This outbreak was caught because of a global early-warning system — the WHO's International Health Regulations framework. The UK reported to WHO on May 2; WHO alerted all member states that same day. That's the system working the way it's supposed to. 12
The US formally exited WHO on January 22, 2026. 3 That means the US is no longer plugged into the real-time IHR intelligence system. The CDC issued its own health advisory independently and deployed a team, so the domestic response happened — but Dr. Carlos del Rio at Emory University noticed something: "I would envision that by now — many, many days ago — we would have seen a team from CDC deployed to the area, and we haven't seen that." 4
The day before the hantavirus alert went out — May 1 — WHO negotiators left Geneva without finalizing the PABS annex of the pandemic treaty, the operational mechanism that would have activated coordinated global vaccine sharing in a future outbreak. The framework exists on paper; the mechanism to use it doesn't. 12
And Dr. Peter Hotez at Baylor College of Medicine framed the longer arc clearly: "We have to be aware of the fact that zoonotic spillover epidemics are increasing with frequency and overall in severity. And this won't be the last one." 13
Hantavirus isn't the next COVID. But it's a real reminder that the conditions for novel outbreaks — habitat disruption, cross-species contact, insufficient surveillance infrastructure, underfunded tropical disease research — are getting worse, not better.
For you specifically, right now: check your notifications, put your phone down, and stop worrying about getting hantavirus. Do spend a few minutes thinking about whether you're up to date on the things that actually matter for people your age — measles vaccine (yes, it's surging again), HIV testing, HPV vaccine if you haven't finished the series. Those are the diseases with real daily risk in your demographic. Hantavirus is not on that list.
참고 출처
- 1WHO Disease Outbreak Notice DON599, May 4 2026
- 2BBC News: Last passengers leave virus-hit cruise ship
- 3CDC Health Alert Network HAN-00528, May 8 2026
- 4NPR: Is hantavirus the next COVID?
- 5CDC: About Andes Virus
- 6JHU Hub: What we know about the hantavirus outbreak
- 7UC Davis Health: Expert Q&A on hantavirus
- 8SAN.com: Hantavirus is not the new COVID-19
- 9Nature: There is no vaccine for deadly hantavirus
- 10NBC News: Scientists are working on a hantavirus vaccine
- 11Bloomberg: Moderna hantavirus efforts underway
- 12El País: WHO faces deadlock over pandemic treaty
- 13USA Today: With fears of hantavirus outbreak, here's the real pandemic risk
이 콘텐츠를 둘러싼 관점이나 맥락을 계속 보강해 보세요.